Last Updated: January 2026
Finding clumps of hair on your pillow, watching strands swirl down the shower drain, or noticing your hairbrush fills up faster than usual—excessive hair shedding is alarming. While it’s completely normal to lose 50-100 hairs daily as part of your hair’s natural growth cycle, anything beyond this can signal an underlying issue that needs attention.
The encouraging news? In most cases, excessive hair shedding is temporary and reversible when you identify and address the root cause. This comprehensive guide combines medical expertise, scientific research, and proven strategies to help you understand why hair sheds excessively and, most importantly, how to stop it.
Understanding Hair Shedding vs. Hair Loss: What’s the Difference?
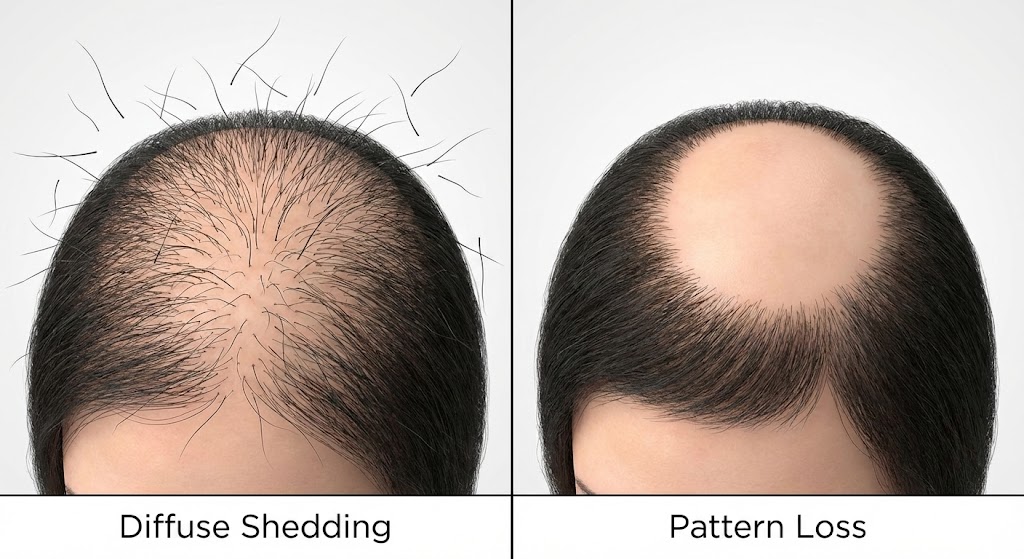
Before diving into solutions, it’s crucial to distinguish between hair shedding and hair loss—they’re not the same condition.
Hair Shedding (Telogen Effluvium)
What it is: Temporary, excessive shedding where hair falls out from the root but follicles remain intact and capable of regrowing hair.
Characteristics:
- Sudden increase in daily hair fall (150-300+ hairs daily)
- Hair comes out easily when washing or brushing
- Usually triggered by a specific event 2-3 months prior
- Affects hair across the entire scalp (diffuse pattern)
- Completely reversible once trigger is addressed
Common triggers: Stress, illness, surgery, childbirth, rapid weight loss, nutritional deficiencies, medication changes
Hair Loss (Anagen Effluvium or Alopecia)
What it is: Actual loss of hair where follicles stop producing new hair or become permanently damaged.
Characteristics:
- Gradual thinning over months or years
- May create specific patterns (receding hairline, crown thinning)
- Hair follicles may become dormant or destroyed
- Often requires medical intervention for regrowth
- May be permanent without treatment
Common causes: Genetics (pattern baldness), autoimmune conditions (alopecia areata), chemotherapy, scarring conditions
Expert Insight: “Most people who come to my office panicked about ‘hair loss’ are actually experiencing telogen effluvium—temporary shedding. The key difference is that shedding is reversible. Once we identify and eliminate the trigger, hair regrows within 3-6 months without any permanent damage to follicles.” — Dr. Sarah Chen, Board-Certified Dermatologist
This guide focuses primarily on stopping excessive hair shedding, though many strategies also support overall hair health for various conditions.
The Hair Growth Cycle: Why Shedding Happens
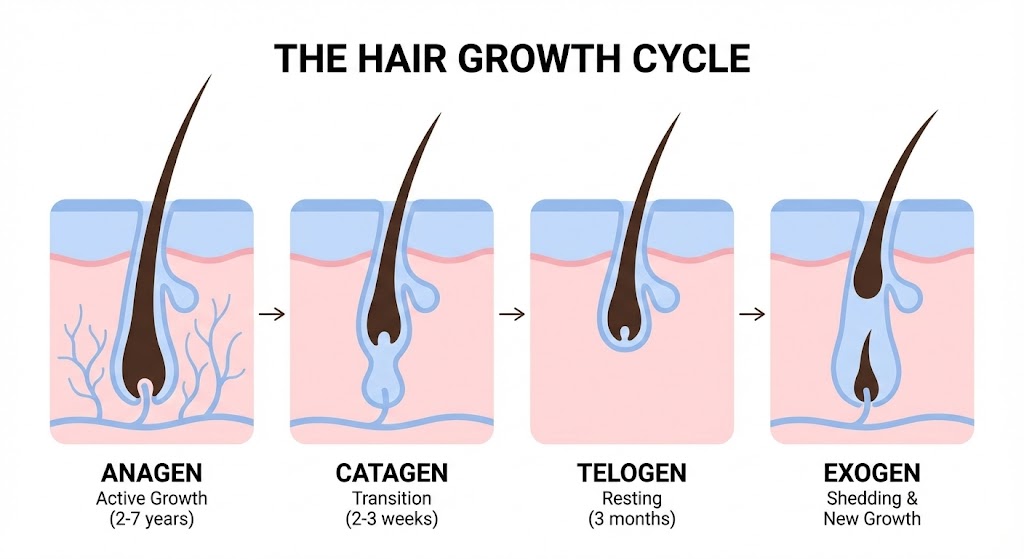
Understanding how hair grows helps explain why shedding occurs and how long recovery takes.
The Four Phases of Hair Growth
1. Anagen Phase (Growth) — 2-7 years
- 85-90% of your hair is in this phase at any time
- Hair actively grows about 6 inches per year
- Longer anagen phase = longer potential hair length
2. Catagen Phase (Transition) — 2-3 weeks
- About 1-2% of hair enters this brief transition
- Hair stops growing as follicle shrinks
- Hair detaches from blood supply
3. Telogen Phase (Rest) — 2-4 months
- Approximately 8-10% of hair is resting
- Hair remains in follicle but isn’t growing
- New hair begins forming beneath resting hair
4. Exogen Phase (Shedding) — 2-5 months
- Old hair sheds to make room for new growth
- 50-100 hairs shed daily during normal exogen
- Shedding can occur during washing, brushing, or spontaneously
What Happens During Excessive Shedding
When you experience a significant stressor (physical or emotional), your body can prematurely push 30-50% of actively growing hairs from anagen into telogen. This creates a synchronized shedding event 2-3 months later when all those hairs enter exogen simultaneously—resulting in dramatic, noticeable hair loss.
Timeline of Telogen Effluvium:
- Month 0: Triggering event occurs (stress, illness, surgery, etc.)
- Months 1-2: Hair quietly enters resting phase (no visible change yet)
- Months 2-4: Massive shedding begins (100-300+ hairs daily)
- Months 3-6: Shedding gradually decreases as new growth begins
- Months 6-12: Hair density returns to normal
Identifying Why Your Hair Is Shedding: Common Causes
Stopping hair shedding requires identifying and addressing the underlying trigger. Here are the most common causes:
1. Chronic or Acute Stress

The Science: Stress hormones (cortisol) disrupt normal hair cycling, forcing growing hairs into premature resting phase. Studies show that psychological stress is one of the leading causes of telogen effluvium.
Types of stress that trigger shedding:
- Emotional stress: Job loss, divorce, death of loved one, financial crisis
- Physical stress: Major surgery, severe illness, car accident, childbirth
- Physiological stress: Crash dieting, extreme exercise, sleep deprivation
Shedding timeline: 2-4 months after stressful event
Solution: Stress management techniques, adequate sleep, counseling if needed
2. Nutritional Deficiencies

The Science: Hair follicles are among the most metabolically active cells in your body, requiring constant nutrient supply. Deficiencies directly impair hair production.
Critical deficiencies that cause shedding:
Iron Deficiency (most common):
- Affects 20% of women, 50% of pregnant women
- Ferritin levels below 40 ng/mL associated with hair loss
- Symptoms: Fatigue, pale skin, brittle nails
Protein Deficiency:
- Hair is 95% keratin (a protein)
- Inadequate protein intake forces body to conserve protein by shutting down hair growth
- Common with crash diets or restrictive eating
Vitamin D Deficiency:
- 40% of Americans are deficient
- Vitamin D receptors in hair follicles essential for cycling
- Levels below 30 ng/mL may contribute to shedding
Zinc Deficiency:
- Critical for hair tissue growth and repair
- Deficiency often seen with digestive disorders or restrictive diets
B-Vitamin Deficiencies (especially B12 and Biotin):
- Essential for red blood cell production (oxygen delivery to follicles)
- Deficiency common in vegetarians/vegans (B12) and certain medications
Solution: Blood testing to identify deficiencies, targeted supplementation, dietary improvements
3. Hormonal Fluctuations
Postpartum Shedding:
- Affects 40-50% of new mothers
- During pregnancy, high estrogen keeps hair in growth phase
- After delivery, estrogen drops dramatically, causing synchronized shedding
- Peaks 3-4 months postpartum
- Resolves naturally by 12 months without treatment
Thyroid Disorders:
- Both hypothyroidism and hyperthyroidism cause diffuse shedding
- Affects hair texture (becoming dry, coarse, or brittle)
- Requires blood testing (TSH, T3, T4) for diagnosis
- Treatment of thyroid condition reverses hair shedding
PCOS (Polycystic Ovary Syndrome):
- Elevated androgens cause pattern thinning on scalp
- May also cause unwanted facial/body hair growth
- Requires hormonal management
Menopause:
- Declining estrogen and progesterone, relative increase in androgens
- Causes gradual thinning and increased shedding
- May require hormone replacement therapy consultation
Solution: Hormone level testing, treatment of underlying hormonal condition, patience during postpartum recovery
4. Medications and Medical Treatments
Common medications that cause hair shedding:
- Blood thinners (heparin, warfarin)
- Antidepressants (some SSRIs)
- Blood pressure medications (beta-blockers, ACE inhibitors)
- Cholesterol-lowering drugs (statins)
- Acne medications (isotretinoin/Accutane)
- Chemotherapy (causes anagen effluvium, not telogen effluvium)
- Birth control pills (when starting or stopping)
Solution: Never stop prescribed medications without consulting your doctor. Discuss alternatives or dosage adjustments if medication is the suspected cause.
5. Underlying Medical Conditions
Conditions associated with excessive shedding:
- Autoimmune disorders (lupus, alopecia areata)
- Iron-deficiency anemia
- Thyroid disease
- Scalp infections (fungal, bacterial)
- Chronic kidney or liver disease
- Eating disorders
- Celiac disease or malabsorption disorders
Solution: Comprehensive medical evaluation, treatment of underlying condition
6. Harsh Hair Care Practices

Physical damage that increases shedding:
Traction Alopecia:
- Caused by tight hairstyles (braids, ponytails, buns, extensions, weaves)
- Constant tension damages follicles over time
- Can become permanent if not corrected early
Heat Damage:
- Excessive blow-drying, flat ironing, curling at high temperatures
- Weakens hair shaft, increasing breakage
- Damaged hair may break before completing growth cycle
Chemical Damage:
- Frequent coloring, bleaching, perming, relaxing
- Damages protein structure of hair
- Weakens hair, making it prone to breakage
Over-washing or Harsh Products:
- Stripping natural oils makes hair brittle
- Sulfates and harsh detergents can irritate scalp
- May accelerate natural shedding process
Solution: Adopt gentle hair care practices, limit chemical and heat styling, avoid tight hairstyles
7. Seasonal Shedding
The phenomenon: Some people experience increased shedding during fall (September-November) and spring.
The science: Research suggests this may be an evolutionary remnant, as many mammals shed seasonally. Studies show telogen rates can increase from 10% to 13% during these periods.
What to do: Seasonal shedding is normal and temporary. If shedding is moderate and resolves within 6-8 weeks, no intervention is needed.
How to Stop Hair Shedding: Proven Strategies
Step 1: Get Professional Diagnosis (Week 1)
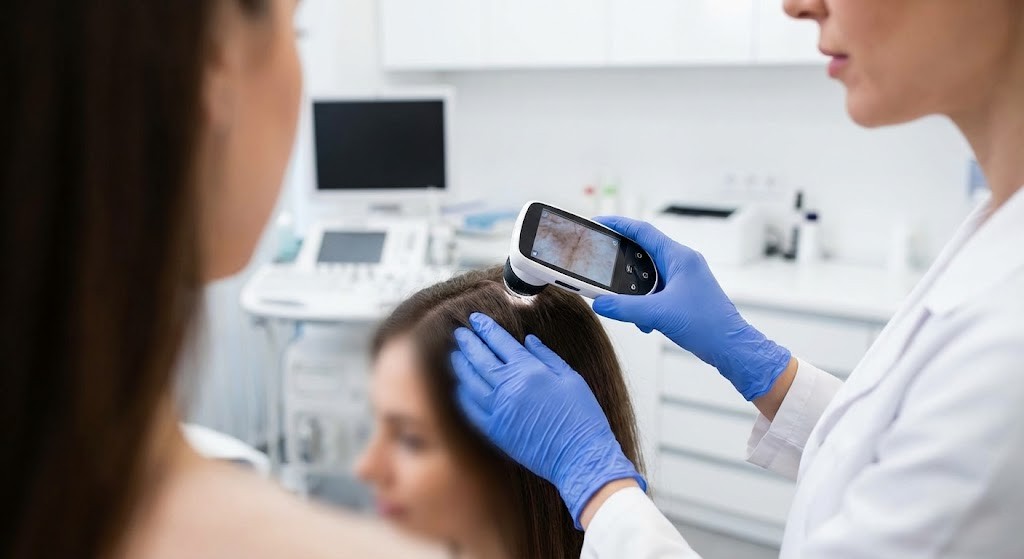
Schedule an appointment with a dermatologist or trichologist who can:
- Perform detailed scalp examination
- Conduct a “pull test” (gently tugging hair to assess shedding severity)
- Order comprehensive blood work:
- Complete blood count (CBC) for anemia
- Ferritin (iron stores) — optimal level 40-70 ng/mL for hair health
- Thyroid panel (TSH, T3, T4)
- Vitamin D, B12
- Zinc levels
- Hormone panels if indicated
- Review medication list for potential culprits
- Possibly perform scalp biopsy if diagnosis unclear
Why this matters: You cannot effectively treat hair shedding without knowing the cause. Blood work often reveals surprising deficiencies even in people who “eat healthy.”
Step 2: Address Nutritional Deficiencies (Weeks 1-4)
If blood work reveals deficiencies, targeted supplementation can dramatically reduce shedding.
Iron Supplementation (if ferritin < 40 ng/mL):
- Dosage: 65-100mg elemental iron daily (with vitamin C for absorption)
- Forms: Ferrous sulfate, ferrous fumarate, or gentler chelated iron
- Timeline: Takes 2-3 months to replenish iron stores
- Side effects: Constipation, nausea (take with food, increase fiber)
- Retest: Check ferritin after 3 months
Vitamin D (if levels < 30 ng/mL):
- Dosage: 2,000-5,000 IU daily depending on deficiency severity
- Best absorbed: With fatty meal
- Timeline: 2-3 months to normalize levels
Biotin:
- Dosage: 2,500-5,000 mcg daily
- Evidence: Limited for hair growth unless deficient, but generally safe
- Note: Can interfere with certain lab tests; inform doctor before blood work
B12 (if deficient, common in vegetarians/vegans):
- Dosage: 1,000 mcg daily or weekly injections for severe deficiency
- Timeline: Several months for improvement
Comprehensive Hair Health Supplement: Consider supplements specifically formulated for hair health containing:
- Biotin (5,000 mcg)
- Iron (if not supplementing separately)
- Zinc (8-11 mg)
- Vitamin E
- Marine collagen or keratin
- Saw palmetto (natural DHT blocker)
Dietary Improvements:
Protein-Rich Foods (aim for 50-60g daily):
- Eggs, fish, chicken, Greek yogurt
- Lentils, chickpeas, quinoa (plant-based options)
Iron-Rich Foods:
- Red meat, spinach, lentils, fortified cereals
- Pair with vitamin C (citrus, tomatoes, bell peppers) for better absorption
- Avoid tea/coffee with iron-rich meals (tannins block absorption)
Omega-3 Fatty Acids:
- Fatty fish (salmon, mackerel, sardines)
- Walnuts, flaxseeds, chia seeds
- Reduces scalp inflammation
Zinc Sources:
- Oysters, beef, pumpkin seeds, chickpeas
Step 3: Optimize Hair Care Routine (Immediate)

Gentle Washing Practices:
Frequency:
- Wash 2-3 times weekly (not daily unless very oily)
- Over-washing strips natural oils; under-washing allows buildup
Technique:
- Use lukewarm water (hot water damages hair)
- Apply shampoo to scalp only, not lengths
- Gently massage scalp with fingertips (not nails)
- Apply conditioner mid-length to ends only (avoid scalp)
- Rinse thoroughly with cool water to seal cuticles
Product Selection:
Choose shampoos with:
- Gentle, sulfate-free cleansers
- Biotin, niacinamide, or caffeine (stimulate follicles)
- Ketoconazole 1-2% (Nizoral) — reduces scalp inflammation and DHT
- Saw palmetto (natural DHT blocker)
Avoid:
- Harsh sulfates (sodium lauryl sulfate)
- Heavy silicones that build up
- Alcohol-based products (drying)
Conditioning:
- Use moisturizing conditioner on lengths
- Consider leave-in conditioner for dry/damaged hair
- Weekly deep conditioning mask
Drying and Styling:
Minimize damage:
- Pat hair dry with microfiber towel or old t-shirt (regular towels create friction)
- Never rub vigorously
- Detangle gently with wide-tooth comb while hair is damp (not soaking wet)
- Air dry when possible
Heat styling:
- Limit to 1-2 times weekly maximum
- Always use heat protectant spray
- Keep tools below 350°F (175°C)
- Never use flat iron on wet hair
Protective practices:
- Sleep on silk or satin pillowcase (reduces friction)
- Loose braid or bun for sleep (not tight ponytail)
- Avoid tight hairstyles during the day
- No hair elastics with metal parts
- Give hair “rest days” from styling
Step 4: Incorporate Scalp-Stimulating Treatments (Weeks 2-4)

Scalp Massage for Blood Flow:
The Science: A 2016 study found that daily 4-minute scalp massages increased hair thickness after 24 weeks by mechanically stretching dermal papilla cells.
Technique:
- Use fingertips (not nails) with medium pressure
- Small circular motions across entire scalp
- 4-5 minutes daily
- Best during shampooing or before bed
Enhanced with oils:
- Add 2-3 drops rosemary or peppermint essential oil to 1 tablespoon carrier oil
- Massage into scalp, leave 30 minutes to overnight
- Shampoo out
Essential Oils with Research Support:
Rosemary Oil:
- 2015 study showed equal effectiveness to 2% minoxidil after 6 months
- Improves circulation, has anti-inflammatory properties
- Mix 5-6 drops in carrier oil (coconut, jojoba, sweet almond)
Peppermint Oil:
- Increases blood flow to follicles
- Studies show increased follicle depth and number (in animals)
- Use same dilution as rosemary
Lavender Oil:
- Promotes hair growth, antimicrobial properties
- Calming scent supports stress reduction
Application method:
- Mix essential oils with carrier oil (never apply undiluted)
- Massage into scalp 2-3x weekly
- Leave minimum 30 minutes or overnight
- Shampoo thoroughly
Topical Treatments:
Minoxidil (Rogaine) 5%:
- FDA-approved for hair loss and excessive shedding
- Extends anagen (growth) phase
- Apply twice daily to dry scalp
- Results in 3-4 months
- Must continue for maintained results
- Over-the-counter availability
Caffeine-Based Products:
- Caffeine stimulates hair follicles
- Available in shampoos and topical solutions
- Less evidence than minoxidil but generally safe
Step 5: Manage Stress Effectively (Ongoing)

Since stress is a primary trigger for telogen effluvium, stress management is essential for both stopping current shedding and preventing future episodes.
Evidence-Based Stress Reduction:
Mindfulness Meditation:
- Benefit: Reduces cortisol (stress hormone) by 20-30%
- How to start: 10 minutes daily using apps like Headspace, Calm, or Insight Timer
- Timeline: Measurable cortisol reduction in 4-8 weeks
Regular Exercise:
- Benefit: Releases endorphins, improves sleep, reduces anxiety
- Recommendation: 30 minutes of moderate activity 5x weekly
- Best options: Walking, swimming, cycling, dancing
- Bonus: Improves blood circulation to scalp
Yoga:
- Benefit: Combines physical activity with stress reduction
- Specific poses: Downward dog, shoulder stand (increase blood flow to scalp)
- Frequency: 2-3 sessions weekly
Professional Support:
- Therapy/Counseling: Particularly helpful for chronic stress, anxiety, depression
- Cognitive Behavioral Therapy (CBT): Evidence-based for stress management
- Support groups: For specific situations (postpartum, grief, chronic illness)
Sleep Optimization:
Why it matters: Sleep deprivation increases cortisol and impairs cellular repair, including hair follicle regeneration.
Sleep hygiene practices:
- Consistent schedule (same bedtime/wake time daily)
- 7-9 hours nightly
- Cool, dark bedroom (65-68°F ideal)
- No screens 1 hour before bed
- Limit caffeine after 2 PM
- Consider magnesium supplement (promotes relaxation)
Step 6: Consider Medical Treatments (If Needed)
When to consider medical intervention:
- Shedding persists beyond 6 months despite lifestyle changes
- Blood work and trigger elimination haven’t helped
- Family history of pattern baldness
- Shedding accompanied by other concerning symptoms
Prescription Options:
Finasteride (Propecia) — Men Only:
- Blocks DHT production
- Primarily for androgenetic alopecia, but may help some telogen effluvium cases
- 1mg daily, prescription required
- Results in 3-6 months
Spironolactone — Women:
- Anti-androgen medication
- Helpful for hormonal hair loss (PCOS, high testosterone)
- Requires monitoring by physician
- Prescription only
Platelet-Rich Plasma (PRP) Therapy:
- Your blood is processed and growth factors injected into scalp
- Stimulates follicle activity
- 3-6 sessions initially, maintenance every 6-12 months
- Cost: $500-$2,000 per session
- Growing evidence for effectiveness
Low-Level Laser Therapy (LLLT):
- FDA-cleared laser caps/combs
- Red light stimulates cellular activity in follicles
- 15-30 minute sessions, 3x weekly
- Results in 3-6 months
- At-home devices: $200-$3,000
Setting Realistic Expectations
Timeline for improvement:
- Weeks 1-8: May see no change or even increased shedding (new hair cycle beginning)
- Months 2-4: Gradual reduction in daily shedding
- Months 4-6: Noticeable decrease in shedding, baby hairs emerging
- Months 6-12: Hair density returns to pre-shedding levels
What success looks like:
- Reduction in hair on pillow, in shower, on brush
- Return to 50-100 hairs shed daily
- New growth visible as short hairs along hairline
- Improved hair texture and strength
Important realities:
- Recovery takes time—hair grows slowly (about 6 inches yearly)
- You must address the root cause, not just symptoms
- Some shedding is always normal (50-100 hairs daily)
- Patience and consistency are essential
Expert Tips for Preventing Future Shedding
Dr. Chen’s Prevention Advice: “Once you’ve experienced telogen effluvium, you’re more susceptible to future episodes. The best prevention is maintaining overall health—manage stress proactively, keep nutrient levels optimal, avoid crash dieting, and be gentle with your hair. Annual blood work can catch deficiencies before they cause shedding. Think of your hair as a health indicator—it often signals problems before other symptoms appear.”
Prevention checklist:
- Annual blood work (ferritin, vitamin D, thyroid, B12)
- Consistent stress management practices
- Balanced diet with adequate protein and nutrients
- Gentle hair care practices always (not just during shedding) Protective styling to prevent traction alopecia
- Adequate sleep (7-9 hours nightly)
- Regular exercise (30 minutes, 5x weekly)
- Immediate action if shedding increases
Remember, hair shedding is usually your body’s way of signaling that something needs attention—stress, nutrition, hormones, or health. By listening to these signals and taking comprehensive action, you can not only stop the shedding but also improve your overall well-being.
The journey starts with that first appointment. Don’t wait until more hair is lost—early intervention produces the fastest, most complete recovery.
Frequently Asked Questions
How long does it take to stop hair shedding?
Most people see significant reduction in shedding within 3-4 months of addressing the underlying cause. Complete recovery typically takes 6-12 months as new hair grows in.
Is it normal to lose 100 hairs per day?
Yes. Losing 50-100 hairs daily is completely normal and part of the natural hair growth cycle. Shedding becomes concerning when you consistently lose 150+ hairs daily.
Can hair shedding be reversed?
Yes, in most cases. Telogen effluvium (temporary shedding) is fully reversible once you identify and address the trigger. Hair follicles remain intact and capable of regrowing hair.
What vitamins stop hair shedding?
No single vitamin “stops” shedding, but correcting deficiencies helps: iron (ferritin 40-70 ng/mL), vitamin D (30+ ng/mL), B12, biotin, and zinc all support hair health. Get blood work to identify your specific deficiencies.
Does stress really cause hair loss?
Absolutely. Stress is one of the most common triggers for telogen effluvium. Both acute stress (surgery, illness, trauma) and chronic stress (work, relationships, anxiety) can push hair into premature shedding phase.
When should I see a doctor for hair shedding? S
See a doctor if you’re losing 150+ hairs daily for more than 2 weeks, notice bald patches, experience scalp symptoms (pain, itching, redness), or if shedding doesn’t improve after 6 months of self-care.
Medical Disclaimer: This article is for informational purposes only and does not constitute medical advice. Hair shedding can indicate underlying health conditions. Always consult with a qualified healthcare provider for proper diagnosis and personalized treatment recommendations.